
If repeated measurements indicate that the fetal heart is deteriorating and that the fetus can no longer survive in utero, the baby will be delivered prematurely by caesarean section. If the fetus is close to term and the complete heart block is considered to be in stable condition, a normal vaginal delivery may be done, but with close monitoring. Treating hydrops in utero with steroids and other drugs may allow the pregnancy to continue and avoid premature delivery, which increases the newborn’s risk of sickness and death. The prognosis is better for fetuses diagnosed with congenital complete heart block without other structural defects of the heart. Fetuses with complete heart block and very low heart rates are at increased risk for development of hydrops. Hydrops, or swelling of the fetus, is an unfavorable sign and is usually associated with a very poor prognosis. The prognosis for these fetuses is guarded, particularly if there are complex malformations.

The outcomes for fetuses diagnosed with congenital complete heart block depend on several factors, but especially significant is whether structural heart disease is also present. Congenital complete heart block usually develops between 18 and 30 weeks gestation. If these studies are normal, obstetricians may continue to follow the fetal heart rate, particularly if the mother previously had a child with complete congenital heart block. Women who know they have antibodies in response to an autoimmune disease should have fetal echocardiography at 18 and at 22 weeks gestation. The heart rate and other measurements of heart function are recorded at the time of diagnosis and usually repeated at intervals of two to four weeks to monitor the condition of the fetal heart. These procedures can also reveal associated problems with the structure of the fetal heart. In fetuses with complete heart block, the rates will not be synchronized. Additional procedures, such as M-mode tracing and Doppler ultrasound can show the relationship between a faster heart rate in the atria and a slower heart rate in the ventricles.
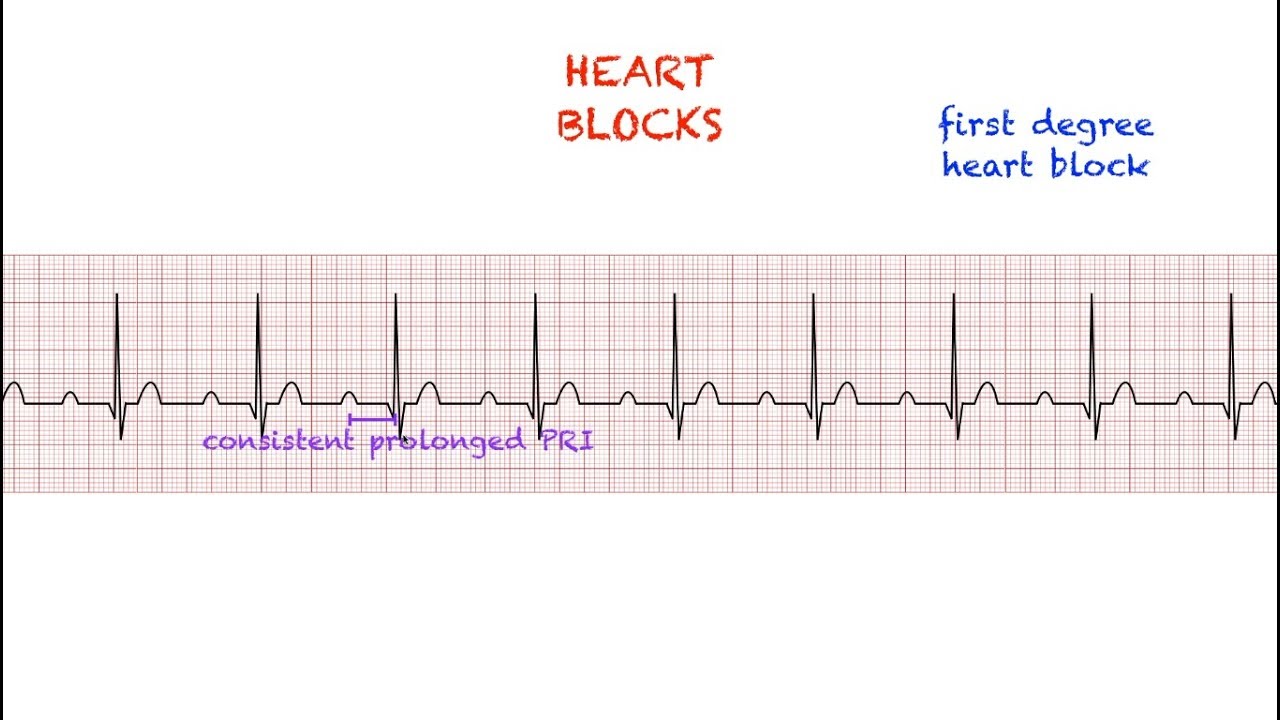
This is known as congenital and can be detected before or after a baby is born.įetal echocardiograms are used to diagnose congenital complete heart block. While all forms of heart block, including complete heart block, more commonly occur after birth, some babies are born with heart block. Also known as complete heart block, third degree is the most severe and represents complete interruption of electrical communication between the atria and ventricles. There are three types of heart block, depending on the extent of disruption of the electrical impulses: first degree, second degree, and third degree. This can limit the ability of the heart to pump blood to the rest of the body. It does mean that the electrical signal that spreads across the heart with each heartbeat is slowed or in some cases completely interrupted. This does not mean that the flow of blood in the heart or that the blood vessels of the heart are blocked. When this signal does not transmit properly, there is heart block or AV block. After the signal passes through the AV node and reaches the ventricles, it causes the heart to contract and pump blood. Normally, the electrical signal passes through specialized conducting tissue known as the atrioventricular (AV) node. Heart block occurs when there is a disruption, preventing the electrical signal from the upper chambers of the heart (the atria) from reaching the lower chambers (the ventricles). Complete heart block is a disorder of the heart’s electrical system, which controls the rate and rhythm of heartbeats.
